Heavy Metal Toxicity in Pets: The Hidden Threat in Your Pet's Environment
An alarming 74% of homes in the United States built before 1980 contain hazardous lead paint, a silent threat lurking in our living spaces [1]. This, coupled with the fact that 17-20% of commercial pet food is co-contaminated with toxic metals, paints a grim picture for our beloved animal companions [2]. Pets, often called the "canaries in the coal mine," serve as sentinel animals for environmental pollution, showing the effects of toxins long before we do [3]. Due to vague and often misleading symptoms, heavy metal toxicity in pets is significantly under-diagnosed. This article will explore the critical topic of heavy metal toxicity, empowering pet owners with the knowledge to recognize, prevent, and address this hidden threat.
Key Takeaways
- Widespread Exposure: 74% of pre-1980 US homes contain lead paint, and 17-20% of commercial pet food is contaminated with heavy metals.
- Vague Symptoms: Signs of toxicity like anorexia, vomiting, and seizures are often non-specific, leading to significant under-diagnosis in pets.
- Age Matters: Younger pets are more susceptible to acute neurological signs, while older pets suffer from cumulative lifetime exposure, facing an 8.97x higher mortality risk in polluted areas.
- Bioaccumulation: Heavy metals like lead, cadmium, and mercury build up in vital organs (brain, liver, kidneys) over time, causing chronic disease and reducing lifespan.
In This Article:
What Are Heavy Metals and Why Are They Dangerous?
Heavy metals are naturally occurring elements characterized by a high atomic weight and density at least 5 times greater than that of water. While some heavy metals are essential for bodily functions in trace amounts (e.g., zinc, copper), others are highly toxic even at very low concentrations.
The "big four" toxic heavy metals of greatest concern for pet health are lead (Pb), cadmium (Cd), mercury (Hg), and arsenic (As) [4]. Unlike nutrients that are metabolized and utilized by the body, these toxic metals bioaccumulate, meaning they build up in living tissues over time because the body lacks the mechanisms to effectively excrete them.
This accumulation primarily occurs in vital organs such as the brain, liver, kidneys, and bones, where they exert their toxic effects through various mechanisms, including oxidative stress, enzyme inhibition, and DNA damage [5]. The cumulative nature of these toxins means that even low-level exposure over a pet's lifetime can lead to a significant toxic burden, with concentrations absorbed in youth becoming clinically significant and potentially life-threatening in old age [6].
Sources of Heavy Metal Exposure in Pets
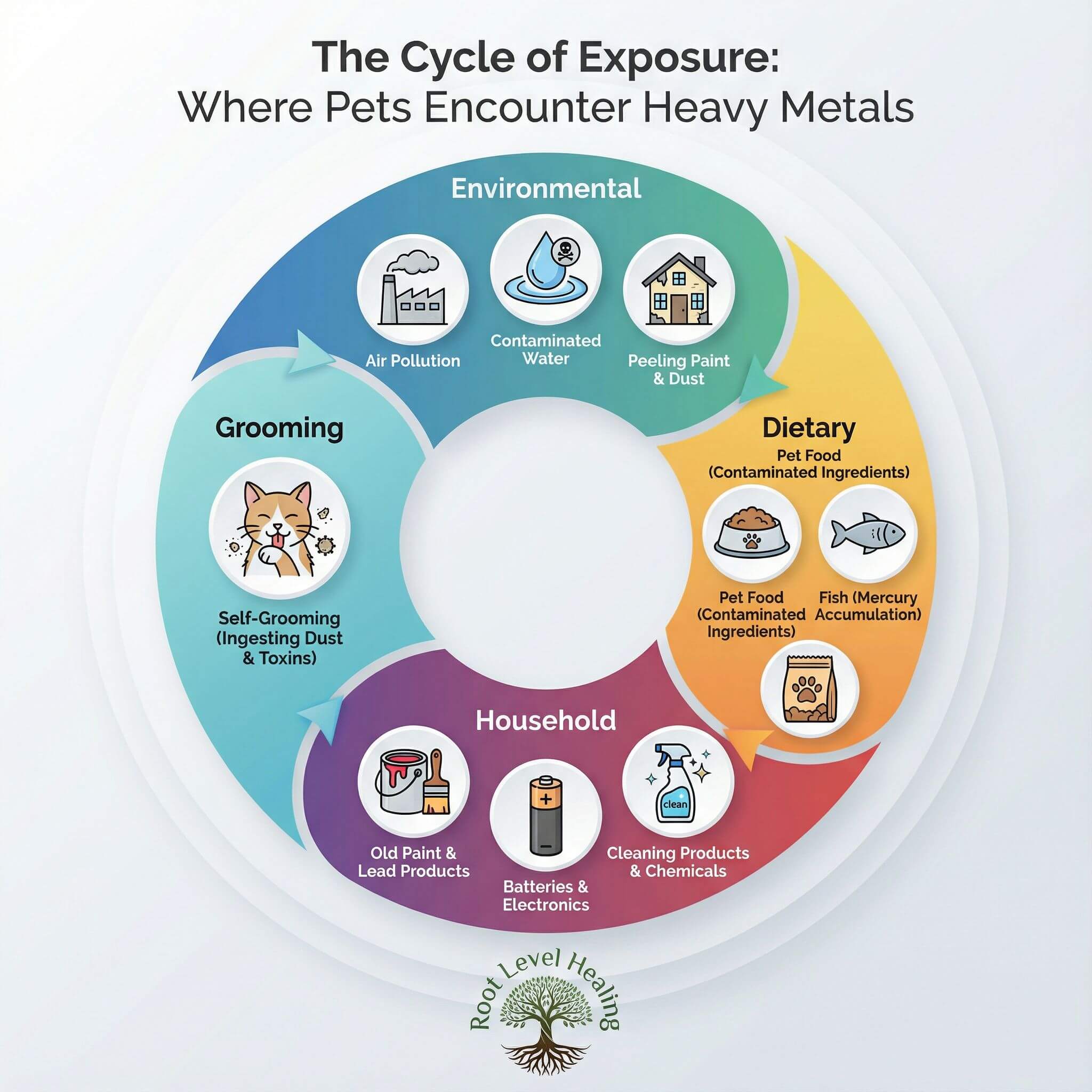
Our pets are exposed to heavy metals from a multitude of sources, often within their own homes and daily routines.
Environmental sources are a major contributor, with old paint being responsible for a staggering 84% of feline lead poisoning cases [1]. Contaminated soil near industrial areas, mines, and highways, as well as air pollution from wildfire smoke and industrial emissions, and even drinking water from old pipes or agricultural runoff, all pose significant risks.
Dietary sources are another major pathway of exposure. Commercial pet food is a significant concern, with studies showing that dry food is more likely to be contaminated than canned food [2]. Fish-based diets have been found to contain higher levels of arsenic, cadmium, and mercury [4]. Even treats and chews, especially imported products, can be a source of contamination.
Household sources further compound the problem. Building materials used during renovations, such as linoleum, caulking, and solder, can release lead dust. Everyday items like pottery glazes, leaded glass artwork, and even automotive products like batteries and used motor oil can be hazardous. Furthermore, the packaging of pet food itself can be a source of toxins, with BPA found in the lining of many pet food cans and PFAS, or "forever chemicals," detected in pet food packaging.
Finally, a pet's own grooming habits can lead to exposure, as cats are particularly vulnerable to ingesting lead dust from their coats and paws after coming into contact with contaminated surfaces.
Common Heavy Metals in Pet Environments
| Heavy Metal | Primary Sources | Target Organs | Toxic Threshold |
|---|---|---|---|
| Lead (Pb) | Old paint, soil, water | Brain, kidneys, GI tract | >30–35 μg/dl blood [1] |
| Cadmium (Cd) | Pet food, industrial emissions | Kidneys, liver, bones | Cumulative [5] |
| Mercury (Hg) | Fish-based diets, environment | Brain, kidneys | Cumulative [5] |
| Arsenic (As) | Pet food, contaminated water | GI tract, skin, liver | Cumulative [4] |
Clinical Signs and Symptoms
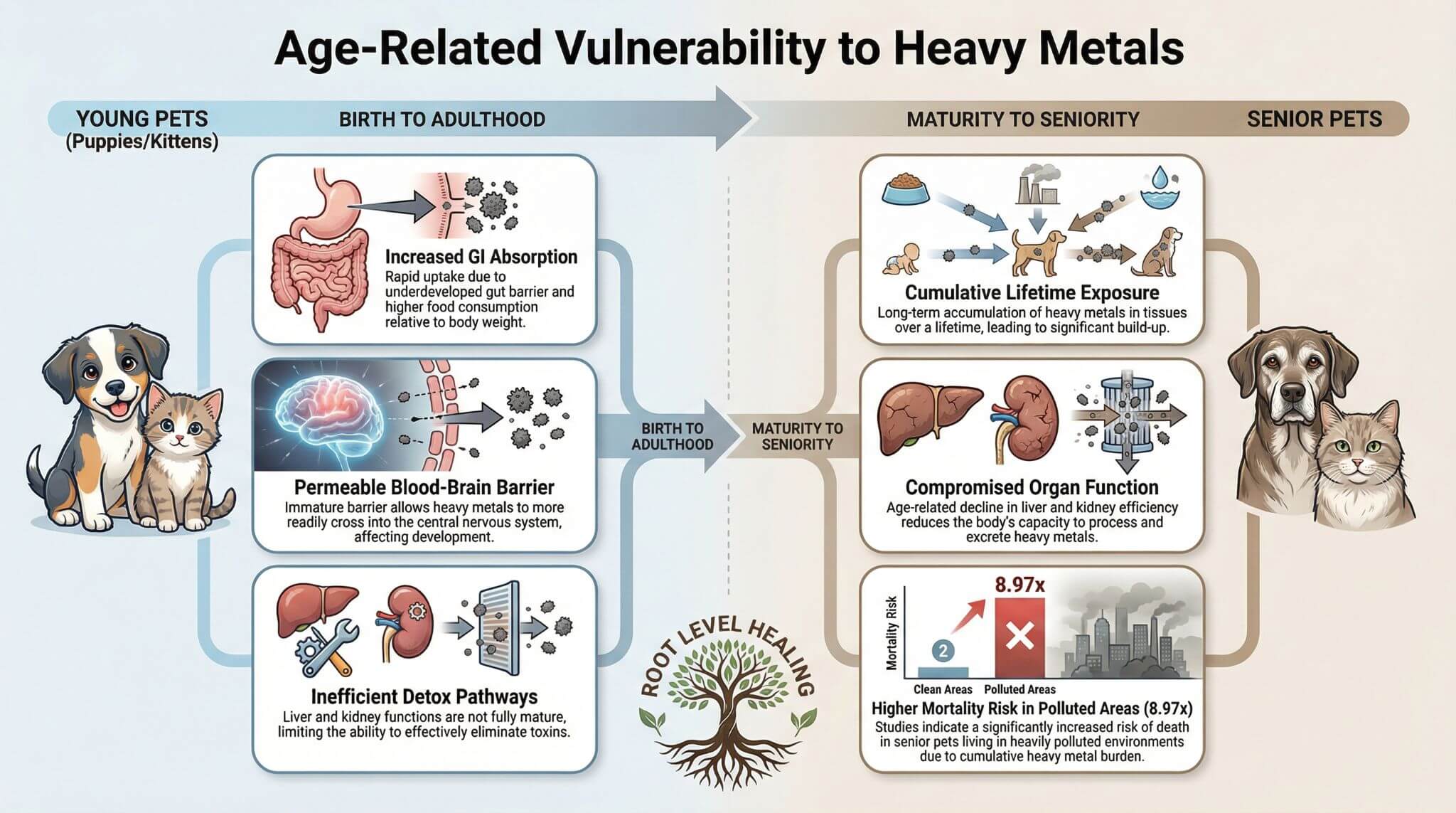
The clinical signs of heavy metal toxicity in pets are often vague and can mimic other common ailments, making diagnosis challenging. A pet's age can influence the presentation of symptoms.
Younger animals, such as puppies and kittens, are more susceptible to neurological signs due to their higher gastrointestinal absorption of lead, a more permeable blood-brain barrier, and less efficient detoxification pathways [1]. In contrast, older animals are more likely to suffer from the cumulative effects of long-term exposure, with one study showing an 8.97 times higher mortality rate in older dogs living in polluted areas [6].
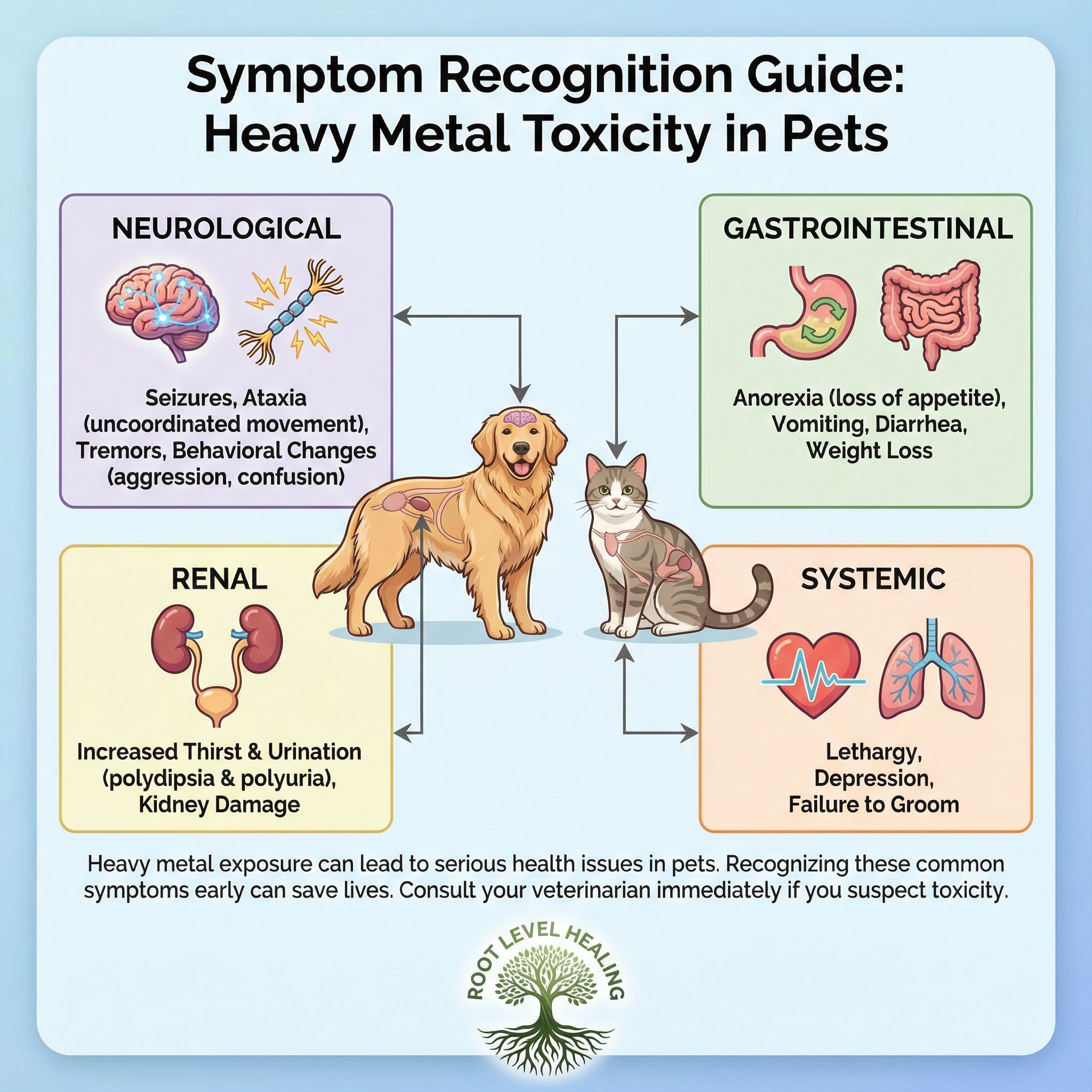
Gastrointestinal signs are among the most common, with anorexia (a loss of appetite) being a primary, and sometimes the only, presenting sign. Vomiting, diarrhea or constipation, colic, abdominal pain, and weight loss are also frequently observed. In some cases, more severe GI issues like megaesophagus can occur.
Neurological signs are particularly concerning and can include seizures, ataxia (loss of coordination), tremors, hyperexcitability, hysteria, blindness, and behavioral changes. Renal signs, such as polyuria/polydipsia (excessive urination and thirst), can indicate renal tubular damage. Systemic signs like lethargy, depression, and failure to groom in cats are also common.
The ambiguity of these symptoms means that heavy metal toxicity is often overlooked, and a high index of suspicion is required for accurate diagnosis.
Heavy Metal Toxicity Symptoms by System
| Body System | Common Symptoms | Severity |
|---|---|---|
| Gastrointestinal | Anorexia, vomiting, diarrhea, weight loss | Mild to Moderate |
| Neurological | Seizures, ataxia, tremors, behavioral changes | Moderate to Severe |
| Renal | Increased thirst/urination, kidney damage | Moderate to Severe |
| Hematological | Anemia, inclusion bodies in blood cells | Mild to Moderate |
📋 Case Study: Luna's Lead Toxicity
Patient: Luna, a 2-year-old domestic shorthair cat
Presentation: Luna's owner brought her to the veterinarian after noticing a 3-week history of decreased appetite, occasional vomiting, and lethargy. The owner had recently begun renovating their 1950s home, removing old paint from window frames.
Diagnosis: Physical examination revealed mild dehydration and a slightly elevated heart rate. Given the history of home renovation and the vague clinical signs, the veterinarian suspected lead toxicity. Blood testing confirmed a blood lead level of 45 μg/dl (normal: <5 μg/dl), well above the toxic threshold of 30-35 μg/dl.
Treatment: Luna was hospitalized for 3 days, receiving intravenous fluids and succimer (DMSA) chelation therapy. The renovation area was sealed off, and the owner implemented lead-safe practices for the remainder of the project.
Outcome: After 14 days of chelation therapy, Luna's blood lead level dropped to 12 μg/dl. Her appetite and energy levels returned to normal within 3 weeks. Follow-up testing at 6 weeks showed a blood lead level of 6 μg/dl, and Luna made a complete recovery. This case highlights the importance of considering environmental factors in diagnosis and the effectiveness of early intervention.
Diagnosis and Testing
Diagnosing heavy metal toxicity requires a combination of clinical suspicion, a thorough history, and confirmatory testing. While blood heavy metal testing is considered the gold standard, it has its limitations.
Blood levels can fluctuate and do not always correlate with the total body burden of the toxin. A pet can have clinical signs of toxicity with normal blood lead levels, and vice versa [1]. Therefore, a diagnosis should not be based solely on blood concentrations.
Other diagnostic tests, such as erythropoietic protoporphyrin (EPP) testing and urine aminolevulinic acid tests, can also be useful. A definitive diagnosis is typically made based on consistent physical examination findings in conjunction with confirmatory test results.
In cases of mortality, necropsy findings can also provide evidence of heavy metal toxicity, with characteristic findings including liver discoloration, the presence of inclusion bodies in liver and renal tissues, and neuronal necrosis in the central nervous system [1].
Treatment and Management
When heavy metal toxicity is diagnosed, prompt and appropriate treatment is essential for the best possible outcome. The treatment approach depends on the severity of exposure, the specific metal involved, and the pet's clinical condition.
Immediate Intervention
The first step in treating heavy metal toxicity is removing the source of exposure. This may involve changing the pet's diet, relocating them away from contaminated environments, or removing hazardous materials from the home. In cases of acute ingestion, such as when a pet has consumed lead paint chips, decontamination procedures like induced vomiting or gastric lavage may be performed under veterinary supervision.
Supportive care is crucial during the treatment process. This includes intravenous fluid therapy to maintain hydration and support kidney function, anticonvulsant medications for pets experiencing seizures, and nutritional support for those with severe gastrointestinal symptoms. Hospitalization may be necessary for pets with severe toxicity to provide intensive monitoring and care.
Chelation Therapy
Chelation therapy is the cornerstone of heavy metal toxicity treatment. Chelating agents are compounds that bind to heavy metals in the body, forming stable complexes that can be excreted through urine or feces. The most commonly used pharmaceutical chelators in veterinary medicine include succimer (DMSA), calcium disodium EDTA, and D-penicillamine.
Succimer (DMSA) is often the first-line chelator for lead toxicity in pets due to its effectiveness and relatively low toxicity profile. It is typically administered orally every 8-12 hours for 10-14 days. Calcium disodium EDTA is another effective chelator, particularly for severe lead poisoning, but requires subcutaneous or intravenous administration and careful monitoring for potential kidney toxicity.
The chelation process must be carefully monitored by a veterinarian, as these medications can have side effects and may require adjustments based on the pet's response. Blood lead levels are typically rechecked after the initial treatment course to determine if additional chelation is needed.
Natural Chelation and Preventive Protocols
For pets with chronic, low-level exposure or as a preventive measure, natural chelation protocols may be recommended. Compounds like orthosilicic acid have been shown to bind heavy metals through ion-exchange mechanisms and support the body's natural detoxification pathways [5]. These natural approaches are generally safer for long-term use and can be integrated into a comprehensive wellness plan.
Nutritional support plays an important role in recovery. Diets rich in antioxidants (vitamins C and E, selenium) can help combat oxidative stress caused by heavy metals. Adequate calcium and iron intake is particularly important, as deficiencies in these minerals can increase the absorption of lead from the gastrointestinal tract.
Prognosis and Recovery
The prognosis for pets with heavy metal toxicity varies depending on several factors, including the type and amount of metal exposure, the duration of exposure, and how quickly treatment is initiated. With early diagnosis and appropriate treatment, many pets make a full recovery, particularly in cases of acute exposure.
Recovery timelines can range from a few weeks for mild cases to several months for more severe toxicity. Neurological symptoms may take longer to resolve, and in some cases, permanent damage may occur if treatment is delayed. Regular follow-up veterinary visits are essential to monitor recovery progress and ensure that blood metal levels return to safe ranges.
The cost of treatment can vary significantly, ranging from $500 to $3,000 or more, depending on the severity of the case and the duration of hospitalization required. Pet insurance may cover some of these costs, making it an important consideration for pet owners in high-risk areas.
When to Seek Veterinary Care
Recognizing when your pet needs immediate veterinary attention can be lifesaving. While heavy metal toxicity often presents with vague symptoms, certain signs warrant urgent evaluation.
Emergency Symptoms
Seek immediate veterinary care if your pet exhibits any of the following emergency symptoms: seizures or convulsions, sudden collapse or inability to stand, severe vomiting or diarrhea lasting more than 24 hours, complete loss of appetite for more than 48 hours, sudden blindness or severe disorientation, or difficulty breathing. These symptoms may indicate severe toxicity requiring immediate intervention.
Non-Emergency but Concerning Signs
Schedule a veterinary appointment within 24-48 hours if your pet shows gradual weight loss over several weeks, persistent lethargy or decreased activity level, intermittent vomiting or diarrhea, behavioral changes such as increased aggression or anxiety, or increased thirst and urination. While these symptoms may not require emergency care, they should not be ignored, especially if your pet has known exposure risks.
Testing After Known Exposure
If you know or suspect your pet has been exposed to heavy metals—such as during home renovations, after ingesting a foreign object, or following a move to an older home—consult your veterinarian about testing even if symptoms are not yet present. Early detection allows for preventive intervention before serious damage occurs. Testing is particularly recommended within 1-2 weeks of suspected exposure for acute incidents, or annually for pets living in high-risk environments.
Long-Term Health Consequences
The cumulative nature of heavy metal toxicity means that long-term exposure can have devastating health consequences for our pets. Studies have shown a 55% higher risk of tumors and a 72% increased risk of lymphoma in dogs living in polluted areas [6].
Chronic kidney disease and neurological damage, including demyelination, are also significant risks [1, 5]. The Italian study on canine mortality highlights the stark reality of this cumulative burden, demonstrating a significantly reduced lifespan for dogs in polluted environments [6].
As biomonitors, our pets often develop these conditions earlier than humans, serving as a poignant indicator of the health of our shared environment [3].
Prevention and Protection Strategies
While the prevalence of heavy metals in our environment can seem overwhelming, there are proactive steps pet owners can take to minimize exposure and protect their pets.
Awareness is the first line of defense. Be mindful of the risks associated with home renovations, especially in older homes, and inquire about lead-safe practices. Choosing high-quality pet food from reputable sources can help reduce dietary exposure. Filtering your pet's drinking water can remove heavy metals and other contaminants.
Regular veterinary check-ups are essential for early detection of any health issues. Minimizing your pet's exposure to contaminated soil and other high-risk areas is also important.
Finally, considering a preventive detoxification protocol can help to reduce the body's toxic burden and support long-term health. These strategies, which will be explored in more detail in our upcoming posts on environmental toxins and the science of detoxification, can make a significant difference in your pet's well-being.
Practical Prevention Guidelines
Implementing specific, actionable prevention strategies can significantly reduce your pet's exposure to heavy metals. Here are detailed recommendations for each area of concern:
Water Filtration
Not all water filters are equally effective at removing heavy metals. Look for filters certified by NSF International for lead reduction (NSF/ANSI Standard 53). Reverse osmosis systems are highly effective at removing lead, cadmium, mercury, and arsenic, typically removing 95-99% of these contaminants. Carbon block filters can also reduce lead levels by 95% or more when properly maintained. Replace filter cartridges according to manufacturer recommendations, as their effectiveness decreases over time.
Pet Food Selection Criteria
When choosing pet food, prioritize brands that conduct third-party testing for heavy metals and publish their results. Look for foods that comply with AAFCO (Association of American Feed Control Officials) standards and have undergone feeding trials. Rotate protein sources rather than feeding exclusively fish-based diets, as fish accumulate mercury and arsenic. Consider brands that source ingredients from regions with stricter environmental regulations. If your pet requires a prescription diet, discuss heavy metal testing options with your veterinarian.
Home Testing and Renovation Safety
If you live in a home built before 1980, consider having your home tested for lead paint using EPA-recognized test kits or hiring a certified lead inspector. During renovations, use EPA Lead-Safe Certified contractors who follow proper containment and cleanup procedures. Keep pets completely out of renovation areas, and thoroughly clean all surfaces with HEPA-filtered vacuums and wet mopping before allowing pets back into renovated spaces. Test your tap water for lead, especially if you have older plumbing, using home test kits or sending samples to certified laboratories.
Soil and Outdoor Environment
Have your yard soil tested if you live near industrial areas, busy roads, or former industrial sites. Soil testing kits are available through university extension services and environmental testing laboratories. If soil contamination is found, create barriers between pets and contaminated soil using raised garden beds, ground covers, or hardscaping. Wipe your pet's paws with pet-safe wipes after outdoor walks, especially in urban areas, to prevent ingestion of contaminants during grooming.
Frequently Asked Questions
Q: How do I know if my pet has heavy metal toxicity?
A: Heavy metal toxicity presents with vague symptoms that can mimic other conditions. Common signs include loss of appetite (anorexia), vomiting, lethargy, weight loss, and in severe cases, seizures or neurological changes. If your pet shows these symptoms, especially after home renovation or known environmental exposure, consult your veterinarian for blood testing.
Q: Are certain pets more vulnerable to heavy metal poisoning than others?
A: Yes, age plays a significant role. Young pets (puppies and kittens) are more susceptible to acute neurological effects due to higher GI absorption and a more permeable blood-brain barrier. Senior pets face higher mortality risk from cumulative lifetime exposure—studies show an 8.97x higher death rate in older dogs living in polluted areas.
Q: Is my pet's food contaminated with heavy metals?
A: Research shows that 17-20% of commercial pet food contains co-contamination with toxic metals like lead, cadmium, mercury, and arsenic. Dry food tends to have higher contamination rates than canned food, and fish-based diets contain significantly higher levels of arsenic, cadmium, and mercury. Choose high-quality brands that conduct third-party testing.
Q: Can heavy metal toxicity be treated?
A: Yes, with early diagnosis and intervention, the prognosis is often good. Treatment involves removing the exposure source, decontamination, supportive care, and chelation therapy. Veterinarians may use pharmaceutical chelators like succimer (DMSA) for acute poisoning, or recommend natural chelation protocols for preventive detoxification.
Q: Should I be worried if I live in an older home?
A: Yes, 74% of US homes built before 1980 contain hazardous lead paint. During renovations, lead dust can contaminate surfaces that pets walk on and then lick during grooming. If you're renovating an older home, keep pets away from work areas, use lead-safe practices, and consider having your pet tested for lead exposure.
Q: What's the difference between acute and chronic heavy metal toxicity?
A: Acute toxicity occurs from sudden, high-level exposure (like ingesting lead paint chips) and causes dramatic symptoms like seizures and severe vomiting. Chronic toxicity develops from low-level exposure over months or years, causing subtle symptoms like gradual weight loss, decreased energy, and eventual organ damage. Both require veterinary attention.
Q: Can I test my pet for heavy metals at home?
A: No reliable at-home tests exist for heavy metal toxicity in pets. Diagnosis requires veterinary blood testing, which measures blood lead levels (toxic at >30-35 μg/dl) and other metals. Your veterinarian may also recommend additional tests like erythropoietic protoporphyrin (EPP) or urine aminolevulinic acid to confirm diagnosis.
Q: Are indoor pets safe from heavy metal exposure?
A: Not necessarily. Indoor pets are still exposed through contaminated pet food, drinking water from old pipes, household dust containing lead or other metals, BPA in canned food, and air pollution. Cats are particularly vulnerable because their grooming behavior causes them to ingest contaminants from their fur and paws.
Q: What's the best way to prevent heavy metal toxicity in my pet?
A: Prevention involves multiple strategies: choose high-quality, tested pet food; filter drinking water; minimize exposure during home renovations; avoid fish-only diets; keep pets away from contaminated soil; and consider preventive detoxification protocols, especially for aging pets or those in urban/industrial areas.
Q: Do heavy metals cause cancer in pets?
A: Yes, research shows a strong correlation. Dogs living in polluted areas have a 55% higher risk of tumors overall and a 72% increased risk of lymphoma specifically. Heavy metals cause oxidative stress and DNA damage, which can lead to cancer development over time. This makes detoxification particularly important for long-term health.
Q: Can detoxification help my pet if they've already been exposed?
A: Yes, both therapeutic and preventive detoxification can help. For acute exposure, veterinary chelation therapy can remove heavy metals from the body. For chronic, low-level exposure, natural chelation protocols using compounds like orthosilicic acid can help reduce the cumulative toxic burden and support long-term organ health.
Q: How often should I have my pet tested for heavy metals?
A: Testing frequency depends on risk factors. High-risk pets (living in pre-1980 homes, urban areas, or eating fish-based diets) should be tested annually or after known exposure events. For average-risk pets, testing every 2-3 years or when symptoms appear is reasonable. Always test senior pets, as cumulative toxicity increases with age.
References
- Knight TE, Kumar MSA. Lead toxicosis in cats—a review. J Feline Med Surg. 2003;5(5):249-255. https://pubmed.ncbi.nlm.nih.gov/12948499/
- Du J, et al. Individual and combined contamination of the toxic metals in commercial cat and dog food. Sci Rep. 2025. https://www.nature.com/articles/s41598-025-98066-0
- Hegedus C, et al. Pets, Genuine Tools of Environmental Pollutant Detection. Animals (Basel). 2023;13(18):2923. https://www.mdpi.com/2076-2615/13/18/2923
- Kim HT, et al. Arsenic, Cadmium, Lead, Mercury in Dog Foods. Korean J Vet Res. 2018;58(4 ):227-231. Available online
- Sears ME. Chelation: Harnessing and Enhancing Heavy Metal Detoxification. ScientificWorldJournal. 2013;2013:219840. https://www.proquest.com/docview/1428013082
- Giugliano R, et al. Mortality and heavy metals environmental exposure in dogs. Front Vet Sci. 2024;10:1297311. https://www.frontiersin.org/journals/veterinary-science/articles/10.3389/fvets.2023.1297311/full
Ready to Discover Your Score?
This 2-minute quiz is the essential first step to understanding your body’s current toxic load and identifying the root cause of how you feel.
Take The Toxicity QuizExplore More Articles
Dive deeper into topics like detoxification, gut health, and mental clarity on our blog. Knowledge is the key to taking control of your health.
Visit The Blog